Natural Treatment for COVID Long-Haulers: What You Need to Know (2022)
The global prevalence of post-COVID syndrome or long COVID four months after the infection is now estimated at 49% of all patients (Journal of Infectious Diseases, November 2022). About 54% of hospitalized patients had long-hauler symptoms and about 34% of non-hospitalized patients had symptoms. This is a very important point to note i.e. severe disease tend to lead to long COVID as compared to mild disease.
Here’s a quick overview of this post:
- Symptoms of long COVID
- Natural Treatments for long COVID
- FLCCC's I-Recover Protocol
- Ways to boost your recovery at home
Symptoms of Long COVID?
An international study showed that fatigue is the most common long-hauler’s syndrome, affecting 80% of all patients. Post-exertional malaise affects 73%, cognitive dysfunction affects 58%, sensorimotor symptoms such as loss of smell affect 56%, headache affects 54%, and memory issues affect 51% (R). A year after infection, common persistent symptoms include fatigue (reported by 82% of patients), brain fog (written by 67%), and headache (reported by 60%) (R).
Natural Treatments for long COVID
1. Vitamin D
Vitamin D3 is essential for supporting healthy immune system function. It works hand in hand with your body to modulate both innate and adaptive immune responses which regulate everything from reactivity to antigens and pathogens.2. Probiotics
COVID can wreak havoc on the gut microbiome, but research on specific probiotic strains that can best restore balance following the syndrome’s particular damage is in its infancy. Leo Galland, MD, a functional-medicine internist in New York City, is looking into soil-derived bacteria of the genus Bacillus because it may have natural antibiotic properties, though there’s not yet enough data to make specific recommendations.Eating fermented foods, such as sauerkraut, yogurt, kefir, and kimchi, can help fortify and support the gut’s microbiome. And in the event of ongoing gut disturbances, working with a functional-medicine provider to design a well-rounded prebiotic and probiotic protocol can help bring the microbiome back into balance.
3. Zinc
4. Melatonin
Supplementing with 1 - 2 mg of melatonin at bedtime might benefit those whose sleep–wake cycles have become dysregulated with long COVID.
5. Omega-3 fatty acids
6. Vitamin C
7. Quercetin, EGCG and Curcumin
Quercetin appears to bind to the spike protein of the coronavirus, inhibit inflammatory pathways, and block replication of infected cells. It is also antiviral and completely safe. In addition to getting sources of quercetin from diet, long-COVID patients can supplement with 250 - 500 mg a day.
8. N-Acetyl-L-Cysteine (NAC)
NAC is an amino acid that the body uses to create glutathione, the body’s master detoxifier. Glutathione is your master detoxifier and the most powerful free radical scavenger produced by your body.Many COVID-19 patients experience serious blood clots, and NAC counteracts hypercoagulation, as it has both anticoagulant and platelet-inhibiting properties.
Aaron Hartman, MD, founder of the Richmond Integrative and Functional Medicine clinic in Richmond, Va., describes one patient, a 26-year-old woman, whose symptoms — persistent low oxygen and shortness of breath — following a bout of COVID resolved after treatment that included NAC as well as omega-3 fish oil.
“NAC is one of the more important nutrients for people who get shortness of breath with COVID, because of its ability to break down those really, really small blood clots called micro-emboli,” explains Hartman.
9. Resveratrol
Resveratrol is a polyphenol with antioxidant and anti-inflammatory
effects that’s found in red grapes, red wine, peanuts, and some
berries. It’s also available as a supplement.
Leo Galland,
MD, a functional-medicine internist in New York City, has found it to
be particularly helpful in restoring his COVID patients to health.
“Resveratrol has a number of beneficial effects on coronavirus
infection,” he notes. “It supports ACE-2 function, it inhibits the
growth of the deadly MERS coronavirus through multiple mechanisms, and
it diminishes the kind of inflammation associated with coronavirus
infection.”
He recommends long-COVID patients supplement with 200 mg of resveratrol twice a day.
10. Lumbrokinase and Serrapeptase
If you’ve had COVID-19, especially if it was a severe case, be aware that blood clots and heart problems, including heart attack, can occur for 90 days or more. It’s believed that remnants of the virus remain in the nervous system, the lungs, the heart and other organs.If the symptoms include major shortness of breath, cough with blood in it or pain on one side when you take a deep breath, it could be due to a late pulmonary embolism or a blood clot going to the lungs.
A safer and likely equally effective alternative to aspirin is digestive fibrinolytic enzymes like lumbrokinase and serrapeptase. You can alternate between the two enzymes — one day take lumbrokinase and the next take serrapeptase — because you’ll need to be on it for about three months and you can develop a sensitivity to them over time.
Anyone who had COVID-19, especially with significant symptoms, should consider taking digestive fibrinolytic enzymes to be sure you don’t have any clotting. An alternative to determine if clotting is occurring is a test called D-dimer, although it can be pricey. D-dimer is a protein fragment produced by the body when a blood clot dissolves.
It’s typically undetectable or present only at very low levels, buts its level may significantly rise when the body is forming and breaking down blood clots (R). If your d-dimer test is low, then you don’t need to take the enzymes. Likewise, if you had a very mild, cold-like case, of COVID-19, you probably don’t need them.
FLCCC I-Recover Protocol
This protocol has also been used to treat post-vaccine inflammatory
syndromes with similar success. As with all FLCCC Alliance
protocols, the components, doses, and durations will evolve as more
clinical data accumulates.
The I-Recover protocol for long haulers has been updated and
below is their latest version (version 3: Sep 6, 2022).
Do not confuse this I-Recover protocol for long haul COVID with another I-Recover protocol for post-vaccine syndrome that was launched in May 2022, by FLCCC. One is for
post covid long haulers and the other, for post vaccine
syndrome.
Treatment must be individualized according to each patient’s
presenting symptoms and disease syndromes. It is likely that not
all patients will respond equally to the same intervention; a
particular intervention may be life-saving for one patient and
totally ineffective for another. Early treatment is essential;
it is likely that the response to treatment will be attenuated
when treatment is delayed.
First-line treatments (In order of priority; not all
required):
-
Prednisone: 10–15mg daily for 3 weeks. Taper to 10mg for three
days, then 5mg for three days and then stop.
-
Ivermectin: 0.2 - 0.3 mg/kg body weight. (Find a Doctor)
-
Low dose naltrexone (LDN): Begin with 1 mg daily and increase
to 4.5mg as required. May take 2–3 months for full effect.
-
Intermittent daily fasting and/or periodic daily fasts:
Fasting promotes autophagy, the body’s protective mechanism to
remove misfolded, foreign and damaged proteins. It also
promotes mitophagy and the release of stem cells. It is likely
that promoting autophagy will aid in the removal of the spike
protein. NOTE: Hydroxychloroquine inhibits autophagy and
should be avoided in patients undergoing intermittent fasting.
-
Spermidine and/or Resveratrol: These compounds have been
demonstrated to augment autophagy. Wheatgerm, mushrooms,
grapefruit, apples and mango are high natural sources of
spermidine. A bio-enhanced formulation containing
trans-resveratrol from Japanese Knotwood Root appears to have
good bio-availability.
-
Melatonin: 8mg at night (slow release/extended release
preferred) with attention to sleep hygiene. Increase dose from
1mg as tolerated (may cause severe nightmares at high
dosages).
-
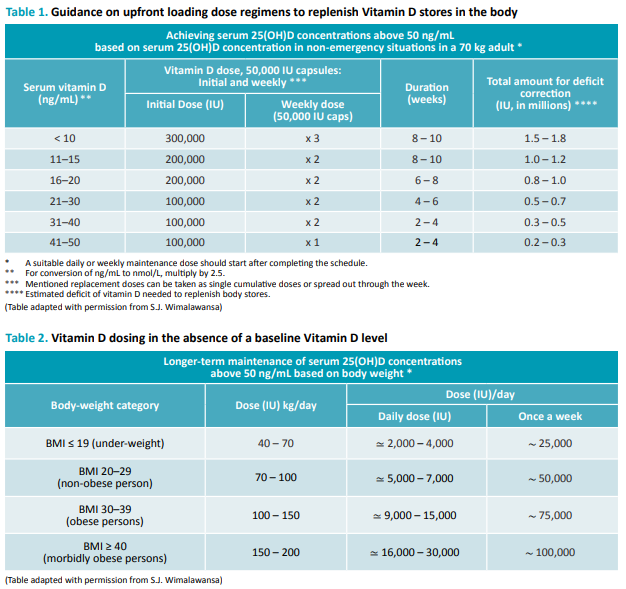
Vitamin D: The majority of those with post-COVID-19 syndrome
continue to have hypovitaminosis D. See tables 1 or 2 for
vitamin D supplementation.
-
Omega-3 fatty acids: Vascepa, Lovaza or DHA/EPA 4g per day.
Omega-3 fatty acids play an important role in the resolution
of inflammation by inducing resolvin production. [Ref, Ref]
-
Curcumin (turmeric): 500 mg twice daily. Has anti-inflammatory
and immunomodulating properties and has been demonstrated to
repolarize macrophages.
- Aspirin — 81 milligrams a day.
2nd Line Therapies
If symptoms do not improve after 1-2 weeks continue steroids,
Omega-3 fatty acids and LDN and add second line therapies as
below.
-
Fluvoxamine (low dose): 25mg once daily. Stop if the symptoms
increase. Caution with the use of other antidepressants and
psychiatric drugs. Taper and discontinue once symptoms
improve.
-
Hydroxychloroquine (HCQ): 200 mg twice daily for 1-2 weeks,
then reduce as tolerated to 200 mg daily. HCQ is the preferred
second line agent. With long term usage, the dose should be
reduced (100 mg or 150 mg daily) in patients weighing less
than 61 kg (135 lbs).
-
Intravenous Vitamin C: 25 g/week, together with oral Vitamin C
1000 mg (1 gram) 2-3 times daily. Oral Vitamin C is important
to provide nutrients for the microbiome. Total daily doses of
8-12 g have been well-tolerated, however chronic high doses
have been associated with the development of kidney stones, so
the duration of therapy should be limited. Wean IV Vitamin C
as tolerated.
-
Mitochondrial energy optimizer with pyrroloquinoline quinone
(e.g., Life Extension Energy Optimizer or ATP 360®).
- N-acetyl cysteine (NAC): 600-1500 mg/day.
3rd Line Therapies
-
Maraviroc (Pfizer’s CCR5 antagonist): 300mg PO
twice a day If 6–8 weeks have elapsed and significant
symptoms persist, consider either getting an InCellDx test
to assess long hauler index profile prior to initiating or
can consider initiating empirically. Note maraviroc can be
expensive and it has risk for significant side effects and
drug interactions.
-
Non-invasive brain stimulation (NIBS): using transcranial
direct current stimulation or transcranial magnetic
stimulation. NIBS is painless, extremely safe, and easy to
administer. NIBS is offered by many Physical Medicine and
Rehabilitation Centers. Patients may also purchase an
FDA-approved device for home use.
The options below are from the I-Recover protocol for long
haulers version 2: Jan 20, 2022. We have included here for your
reference.
Optional adjunctive therapies (in order of priority)
-
Nigella Sativa: which like curcumin has anti-inflammatory
and immunomodulating properties.
-
Atorvastatin: 20–40mg once daily. Caution in patients with
Postural Orthostatic Tachycardia Syndrome (POTS); may
exacerbate symptoms.
-
Kefir, probiotic yogurt and/or Bifidobacterium Probiotics
(e.g., Daily Body Restore) together with Prebiotics (e.g.
XOS Prebiotic, Bio Nutrition Pre-Biotic) to normalize the
microbiome. Prolonged dysbiosis has been reported following
COVID-19 infection.
-
Behavioral modification, mindfulness therapy and
psychological support may help improve survivors’ overall
well-being and mental health.
-
Luteolin 100–200mg day or Quercetin 250mg day (or mixed
flavonoids). Luteolin and quercetin have broad spectrum
anti-inflammatory properties. These natural flavonoids
inhibit mast cells, and have been demonstrated to reduce
neuroinflammation. [R]
-
H1 receptor blockers (for mast cell activation syndrome):
Loratadine 10mg daily, or Cetirizine 5–10mg daily, or
Fexofenadine 180mg — daily.
-
H2 receptor blockers (for mast cell activation syndrome):
Famotidine 20–40mg, or Nizatidine 150mg — twice daily as
tolerated.
-
Montelukast: 10mg/day (for mast cell activation syndrome).
Caution as may cause depression in some patients.
-
Anti-androgen therapy: Spironolactone 50–100mg twice a day,
and Dutasteride 1mg daily.
Mast cell stabilisers: rupadatadine, quercetin or
luteolin.
Ways to boost your recovery at home
- Prednisone: 10–15mg daily for 3 weeks. Taper to 10mg for three days, then 5mg for three days and then stop.
- Ivermectin: 0.2 - 0.3 mg/kg body weight. (Find a Doctor)
- Low dose naltrexone (LDN): Begin with 1 mg daily and increase to 4.5mg as required. May take 2–3 months for full effect.
- Intermittent daily fasting and/or periodic daily fasts: Fasting promotes autophagy, the body’s protective mechanism to remove misfolded, foreign and damaged proteins. It also promotes mitophagy and the release of stem cells. It is likely that promoting autophagy will aid in the removal of the spike protein. NOTE: Hydroxychloroquine inhibits autophagy and should be avoided in patients undergoing intermittent fasting.
- Spermidine and/or Resveratrol: These compounds have been demonstrated to augment autophagy. Wheatgerm, mushrooms, grapefruit, apples and mango are high natural sources of spermidine. A bio-enhanced formulation containing trans-resveratrol from Japanese Knotwood Root appears to have good bio-availability.
- Melatonin: 8mg at night (slow release/extended release preferred) with attention to sleep hygiene. Increase dose from 1mg as tolerated (may cause severe nightmares at high dosages).
- Vitamin D: The majority of those with post-COVID-19 syndrome continue to have hypovitaminosis D. See tables 1 or 2 for vitamin D supplementation.
- Omega-3 fatty acids: Vascepa, Lovaza or DHA/EPA 4g per day. Omega-3 fatty acids play an important role in the resolution of inflammation by inducing resolvin production. [Ref, Ref]
- Curcumin (turmeric): 500 mg twice daily. Has anti-inflammatory and immunomodulating properties and has been demonstrated to repolarize macrophages.
- Aspirin — 81 milligrams a day.
- Fluvoxamine (low dose): 25mg once daily. Stop if the symptoms increase. Caution with the use of other antidepressants and psychiatric drugs. Taper and discontinue once symptoms improve.
- Hydroxychloroquine (HCQ): 200 mg twice daily for 1-2 weeks, then reduce as tolerated to 200 mg daily. HCQ is the preferred second line agent. With long term usage, the dose should be reduced (100 mg or 150 mg daily) in patients weighing less than 61 kg (135 lbs).
- Intravenous Vitamin C: 25 g/week, together with oral Vitamin C 1000 mg (1 gram) 2-3 times daily. Oral Vitamin C is important to provide nutrients for the microbiome. Total daily doses of 8-12 g have been well-tolerated, however chronic high doses have been associated with the development of kidney stones, so the duration of therapy should be limited. Wean IV Vitamin C as tolerated.
- Mitochondrial energy optimizer with pyrroloquinoline quinone (e.g., Life Extension Energy Optimizer or ATP 360®).
- N-acetyl cysteine (NAC): 600-1500 mg/day.
- Maraviroc (Pfizer’s CCR5 antagonist): 300mg PO twice a day If 6–8 weeks have elapsed and significant symptoms persist, consider either getting an InCellDx test to assess long hauler index profile prior to initiating or can consider initiating empirically. Note maraviroc can be expensive and it has risk for significant side effects and drug interactions.
- Non-invasive brain stimulation (NIBS): using transcranial direct current stimulation or transcranial magnetic stimulation. NIBS is painless, extremely safe, and easy to administer. NIBS is offered by many Physical Medicine and Rehabilitation Centers. Patients may also purchase an FDA-approved device for home use.
- Nigella Sativa: which like curcumin has anti-inflammatory and immunomodulating properties.
- Atorvastatin: 20–40mg once daily. Caution in patients with Postural Orthostatic Tachycardia Syndrome (POTS); may exacerbate symptoms.
- Kefir, probiotic yogurt and/or Bifidobacterium Probiotics (e.g., Daily Body Restore) together with Prebiotics (e.g. XOS Prebiotic, Bio Nutrition Pre-Biotic) to normalize the microbiome. Prolonged dysbiosis has been reported following COVID-19 infection.
- Behavioral modification, mindfulness therapy and psychological support may help improve survivors’ overall well-being and mental health.
- Luteolin 100–200mg day or Quercetin 250mg day (or mixed flavonoids). Luteolin and quercetin have broad spectrum anti-inflammatory properties. These natural flavonoids inhibit mast cells, and have been demonstrated to reduce neuroinflammation. [R]
- H1 receptor blockers (for mast cell activation syndrome): Loratadine 10mg daily, or Cetirizine 5–10mg daily, or Fexofenadine 180mg — daily.
- H2 receptor blockers (for mast cell activation syndrome): Famotidine 20–40mg, or Nizatidine 150mg — twice daily as tolerated.
- Montelukast: 10mg/day (for mast cell activation syndrome). Caution as may cause depression in some patients.
- Anti-androgen therapy: Spironolactone 50–100mg twice a day, and Dutasteride 1mg daily.
Ways to boost your recovery at home
Follow a Balanced Diet
If you’re experiencing the effects of long COVID, what you eat will have a major impact on how you feel. Choosing to follow a healthy and balanced diet is a good way to promote your recovery at home.
Some foods, such as oily fish rich in omega-3, nuts, and seeds, can be helpful to reduce the inflammatory response characteristic of this viral disease. Also, fruit and vegetables are high in antioxidants and can counteract oxidative stress caused by inflammation. In contrast, you should avoid foods like highly processed foods, high in fat or high in sugar, as these may have a pro-inflammatory effect.
Rest Frequently during the Day
Patients often find that attempts to push through fatigue and migraines make them feel worse and exacerbate the intensity of their symptoms. While you’re recovering, rest as much as you need, and allow yourself more time to complete your normal routine. Pace yourself during the day. Carefully plan what you need to do but don’t overexert yourself. Take breaks when needed.
Break complex or time-consuming tasks into smaller chunks and alternate between easy and difficult activities.
Pick the time of the day when you’re more alert to complete the most important or difficult tasks.
Practice breathing exercises to control your breathing patterns and relax both body and mind.
Follow a Good Sleep Pattern
Studies show that up to half of long haulers complain of sleep disorders. This is not surprising as sleep patterns can be disrupted after a viral infection. If you have trouble falling asleep or wake up frequently during the night, it’s important that you address this issue. There is a close relationship between poor sleep and poor mental health. A poor night’s sleep can make feelings of depression, anxiety, and stress feel worse.Go to bed early and follow the same pattern every day.
Avoid screens close to bedtime and use blue-light filters when you do use them.
Restrict caffeine to the morning only (although it’s better if you can do without it while you recover). Avoid alcohol at night as well.
Make sure your bedroom has a relaxing atmosphere that can help you sleep. You might need to declutter or add a source of white noise.
If you need it, take a short nap during the day, but no longer than 30 minutes. Longer naps can actually be counterproductive.
Engage in Regular Exercise
Physical activity plays a vital role during recovery from long COVID. Choose something that you can achieve without causing a massive flare-up of your long-haul symptoms. There’s a fine balance between doing too much and not doing enough. We highly recommend intervals: Short bursts of cardio (around 30 seconds to one minute) followed by one to two minutes of controlled breathing.
To know when it’s safe to continue exercising versus when you should stop, follow this simple rule:If you’ve noticed three symptoms starting or getting worse during exercise, then it’s time to stop.
Similarly, if a single symptom is getting worse quickly, going from what you would rate as a 1 (mild) to a 4 (severe), it’s a sign that you need a break.
If you’re just feeling a slight headache or experiencing mild dizziness, it’s okay to continue. Exercise helps the brain heal and will keep other symptoms under control in the future.
Reduce Stress in Your Life
Dealing with long COVID can be very stressful. As you’re able, plan some “you” time during the day. Go for a walk, sign up for a yoga class, or simply sit in a quiet place reading a good book. Learn your symptom triggers and avoid or limit situations that may push you past your limits. For example, if driving in heavy traffic is too much for you, look for an alternative route or travel at a different time.
You may find it helpful to stick to a consistent daily routine. And don’t be afraid to ask loved ones for help when you need it.
Remember that some days will be better than others. Recovery isn’t linear, but you can keep improving with time.
- For treatment of post-vaccine syndrome, check out i-Recover Post Vaccine Treatment Protocol.
- Find health care providers: FIND A DOCTOR WHO WILL PRESCRIBE IVERMECTIN, HYDROXYCHLOROQUINE AND EARLY OUTPATIENT TREATMENTS FOR COVID-19 (USA)
- For comprehensive reviews on topics and research regarding long COVID, check out this long COVID video series by Dr Been.
- Post-COVID recovery clinics are being launched nationwide in U.S. to address this still-growing need.





.png)

Comments
Post a Comment